There are high number of clear evidence that breastfeeding provides best nutrition that you can give to your baby. It is also evident that lactation is good for mothers health as well. Evolution has designed breastfeeding in a way that it caters all nutritional need of your child. However modern medicine is quite new for evolution, that is why mothers body is not well prepared to filter unnecessary chemical found in medicines. It becomes a necessity to figure out which drug is safe and which drug is dangerous for your newborn while nursing. In this article we will understand function of Valsartan And Hydrochlorothiazide Tablet and its suitability with breastfeeding.
What is Valsartan And Hydrochlorothiazide Tablet used for?
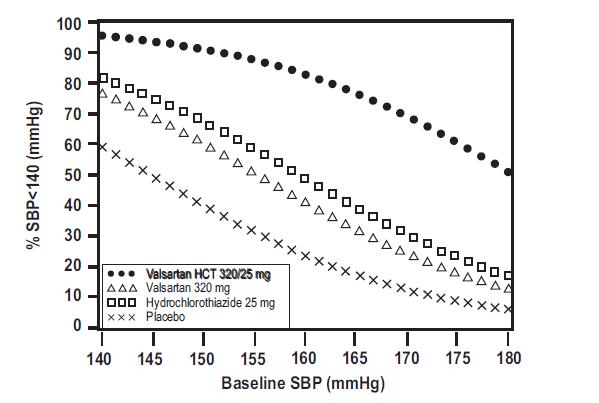
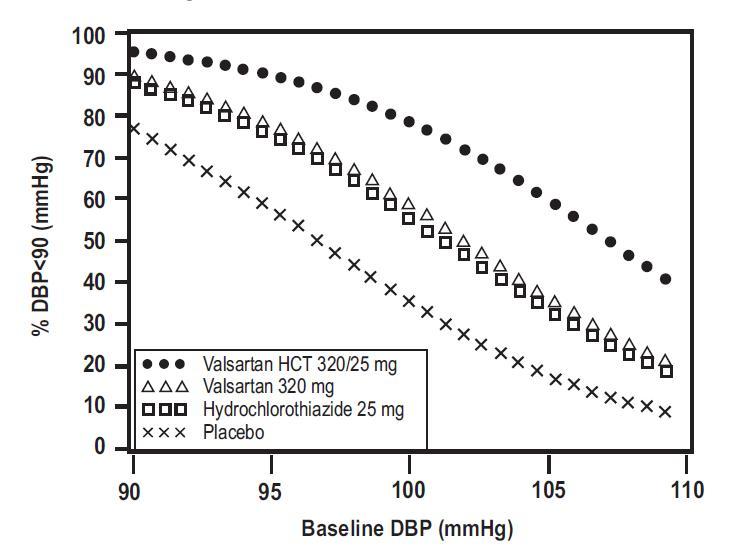
Valsartan and hydrochlorothiazide tablets, USP are indicated for the treatment of hypertension, to lower blood pressure. Lowering blood pressure reduces the risk of fatal and nonfatal cardiovascular events, primarily strokes and myocardial infarctions. These benefits have been seen in controlled trials of antihypertensive drugs from a wide variety of pharmacologic classes, including hydrochlorothiazide and the ARB class to which valsartan principally belongs. There are no controlled trials demonstrating risk reduction with valsartan and hydrochlorothiazide tablets, USP. Control of high blood pressure should be part of comprehensive cardiovascular risk management, including, as appropriate, lipid control, diabetes management, antithrombotic therapy, smoking cessation, exercise, and limited sodium intake. Many patients will require more than 1 drug to achieve blood pressure goals. For specific advice on goals and management, see published guidelines, such as those of the National High Blood Pressure Education Program’s Joint National Committee on Prevention, Detection, Evaluation, and Treatment of High Blood Pressure (JNC). Numerous antihypertensive drugs, from a variety of pharmacologic classes and with different mechanisms of action, have been shown in randomized controlled trials to reduce cardiovascular morbidity and mortality, and it can be concluded that it is blood pressure reduction, and not some other pharmacologic property of the drugs, that is largely responsible for those benefits. The largest and most consistent cardiovascular outcome benefit has been a reduction in the risk of stroke, but reductions in myocardial infarction and cardiovascular mortality have also been seen regularly. Elevated systolic or diastolic pressure causes increased cardiovascular risk, and the absolute risk increase per mmHg is greater at higher blood pressures, so that even modest reductions of severe hypertension can provide substantial benefit. Relative risk reduction from blood pressure reduction is similar across populations with varying absolute risk, so the absolute benefit is greater in patients who are at higher risk independent of their hypertension (for example, patients with diabetes or hyperlipidemia), and such patients would be expected to benefit from more aggressive treatment to a lower blood pressure goal. Some antihypertensive drugs have smaller blood pressure effects (as monotherapy) in black patients, and many antihypertensive drugs have additional approved indications and effects (e.g., on angina, heart failure, or diabetic kidney disease). These considerations may guide selection of therapy. Add-On Therapy Valsartan and hydrochlorothiazide tablets, USP may be used in patients whose blood pressure is not adequately controlled on monotherapy. Replacement Therapy Valsartan and hydrochlorothiazide tablets, USP may be substituted for the titrated components. Initial Therapy Valsartan and hydrochlorothiazide tablets, USP may be used as initial therapy in patients who are likely to need multiple drugs to achieve blood pressure goals. The choice of valsartan and hydrochlorothiazide tablets, USP as initial therapy for hypertension should be based on an assessment of potential benefits and risks. Patients with stage 2 hypertension are at a relatively high risk for cardiovascular events (such as strokes, heart attacks, and heart failure), kidney failure, and vision problems, so prompt treatment is clinically relevant. The decision to use a combination as initial therapy should be individualized and should be shaped by considerations such as baseline blood pressure, the target goal and the incremental likelihood of achieving goal with a combination compared to monotherapy. Individual blood pressure goals may vary based upon the patient's risk. Data from the high dose multifactorial trial [see Clinical Studies ( 14.1)] provides estimates of the probability of reaching a target blood pressure with valsartan and hydrochlorothiazide tablets, USP compared to valsartan or hydrochlorothiazide monotherapy. The figures below provide estimates of the likelihood of achieving systolic or diastolic blood pressure control with valsartan and hydrochlorothiazide tablets, USP 320/25 mg, based upon baseline systolic or diastolic blood pressure. The curve of each treatment group was estimated by logistic regression modeling. The estimated likelihood at the right tail of each curve is less reliable due to small numbers of subjects with high baseline blood pressures. Figure 1: Probability of Achieving Systolic Blood Pressure <140 mmHg at Week 8 Figure 2: Probability of Achieving Diastolic Blood Pressure <90 mmHg at Week 8 Figure 3: Probability of Achieving Systolic Blood Pressure <130 mmHg at Week 8 Figure 4: Probability of Achieving Diastolic Blood Pressure <80 mmHg at Week 8 For example, a patient with a baseline blood pressure of 160/100 mmHg has about a 41% likelihood of achieving a goal of <140 mmHg (systolic) and 60% likelihood of achieving <90 mmHg (diastolic) on valsartan alone and the likelihood of achieving these goals on HCTZ alone is about 50% (systolic) or 57% (diastolic). The likelihood of achieving these goals on valsartan and hydrochlorothiazide tablets, USP rises to about 84% (systolic) or 80% (diastolic). The likelihood of achieving these goals on placebo is about 23% (systolic) or 36% (diastolic). Valsartan and hydrochlorothiazide tablets, USP are the combination tablet of valsartan, an angiotensin II receptor blocker (ARB) and hydrochlorothiazide (HCTZ), a diuretic. Valsartan and hydrochlorothiazide tablets, USP are indicated for the treatment of hypertension, to lower blood pressure : • In patients not adequately controlled with monotherapy ( 1) • As initial therapy in patients likely to need multiple drugs to achieve their blood pressure goals ( 1) Lowering blood pressure reduces the risk of fatal and nonfatal cardiovascular events, primarily strokes and myocardial infarctions figure-1 figure-2 figure-3 figure-4
What are the risk associated with Valsartan And Hydrochlorothiazide Tablet usage while breastfeeding? What precautions shall I take while using it in breastfeeding?
Valsartan and Hydrochlorothiazide are the two main ingredients of Valsartan And Hydrochlorothiazide Tablet. Based on our individual analysis of Valsartan and Hydrochlorothiazide we can safely say that Valsartan And Hydrochlorothiazide Tablet has low risk while breastfeeding. Below we have summarized the usage of Valsartan and Hydrochlorothiazide while breastfeeding, we recommend you to go through it for better understanding of your usage.
Statement of Manufacturer/Labeler about breastfeeding usage
8.3 Nursing Mothers It is not known whether valsartan is excreted in human milk. Valsartan was excreted into the milk of lactating rats; however, animal breast milk drug levels may not accurately reflect human breast milk levels. Hydrochlorothiazide is excreted in human breast milk. Because many drugs are excreted into human milk and because of the potential for adverse reactions in nursing infants from valsartan and hydrochlorothiazide tablets, a decision should be made whether to discontinue nursing or discontinue the drug, taking into account the importance of the drug to the mother.
Valsartan And Hydrochlorothiazide Tablet Breastfeeding Analsys
Low RiskCAS Number: 137862-53-4
At latest update, relevant published data on excretion into breast milk were not found. A high protein-binding capacity makes excretion into breast milk unlikely. In addition, a low oral bioavailability makes difficult the absorption towards the infant's plasma from ingested milk, except in prematures or newborns who may show an increased absorption. Case report of kidney function impairment of a baby whose mother had taken Telmisartan in pregnancy. Until more data on this medication is available, safer alternative drugs are preferred, especially in premature babies or during the neonatal period. Should an ARA-II medication (Sartan type) be necessary, the associated risk may be decreased by choosing the one with a favorable pharmacokinetics (shorter half-life elimination time and lower bioavailability) like Eprosartan and Losartan
SafeCAS Number: 58-93-5
Thiazide diuretic drug. Excretion into breast milk is clinically non-significant. No side-effects were observed in a one-month old breastfed baby whose mother was treated with this medication. Drug level in the plasma of this child was undetectable. Long-term treatment with diuretic drugs (particularly Thiazide type ones with long-lasting effect and loop-acting mechanism) may inhibit lactation, mostly if lactation is not well-established yet. Use as lower dose as possible, especially during the first postnatal month. American Academy of Pediatrics 2013: Maternal Medication Usually Compatible With Breastfeeding. WHO Model List of Essential Drugs 2002: Compatible with breastfeeding.
Valsartan And Hydrochlorothiazide Tablet Breastfeeding Analsys - 2
CAS Number: 137862-53-4
Because no information is available on the use of valsartan during breastfeeding, an alternate drug may be preferred, especially while nursing a newborn or preterm infant.
CAS Number: 58-93-5
Hydrochlorothiazide doses of 50 mg daily or less are acceptable during lactation. Intense diuresis with large doses may decrease breastmilk production.
What should I do if I am breastfeeding mother and I am already exposed to Valsartan And Hydrochlorothiazide Tablet?
During whole lactation period you shall first discuss with your doctor and then together you shall decide whether you shall take that drug or not however if you have already taken Valsartan And Hydrochlorothiazide Tablet then you shall inform your doctor, But you should not be worried too much as Valsartan And Hydrochlorothiazide Tablet comes in category of low risk drug.
I am nursing mother and my doctor has suggested me to use Valsartan And Hydrochlorothiazide Tablet, is it safe?
Valsartan And Hydrochlorothiazide Tablet comes in category of low risk and if your doctor is aware that you are breastfeeding it should be ok to use without much concerns.
If I am using Valsartan And Hydrochlorothiazide Tablet, will my baby need extra monitoring?
Not much
Who can I talk to if I have questions about usage of Valsartan And Hydrochlorothiazide Tablet in breastfeeding?
US
National Womens Health and Breastfeeding Helpline: 800-994-9662 (TDD 888-220-5446) 9 a.m. and 6 p.m. ET, Monday through Friday
UK
National Breastfeeding Helpline: 0300-100-0212 9.30am to 9.30pm, daily
Association of Breastfeeding Mothers: 0300-330-5453
La Leche League: 0345-120-2918
The Breastfeeding Network supporter line in Bengali and Sylheti: 0300-456-2421
National Childbirth Trust (NCT): 0300-330-0700
Australia
National Breastfeeding Helpline: 1800-686-268 24 hours a day, 7 days a week
Canada
Telehealth Ontario for breastfeeding: 1-866-797-0000 24 hours a day, 7 days a week
Drug Brands with same Active ingredients




